Getting Nursing Home Care Right
Pioneer Institute has long recognized that seniors deserve the best of care and that innovative policy solutions are necessary to ensure that this population enjoys a high quality of life in their later years. In the 1990s, early 2000s and most recently in 2017, the Institute dedicated Better Government Competition topics to policy issues related to aging in America. Our goal each time was to find solutions and to take advantage of new innovations that would improve the quality of life and care for the elderly.
COVID-19 has hurled intense, disproportionate and deadly challenges at seniors and their caregivers. Since the beginning of the pandemic surge in Massachusetts, Pioneer expanded its focus on nursing homes and the response of the Commonwealth to contain COVID-19 spread among seniors. We have looked at both the lack of state transparency and the substance of measures taken to contain spread. In both cases, transparency and substance, Pioneer found the Commonwealth’s response inadequately protected those in the vulnerable circumstances of long-term care facilities.
Some of our key recommendations include:
- Oversight: Pioneer called on leaders to appoint an individual (preferably a public health expert, epidemiologist, or virologist) with sole responsibility for oversight and coordination of the responses of state agencies and nursing homes, reporting directly to the Governor.
- Transparency: Pioneer called for increased public accessibility of data, including disclosure of COVID-19 case and death totals in absolute numbers by facility, and disclosure of whether a nursing home is accepting COVID-19 patients from hospitals.
- Equipment: Pioneer recommended requiring nursing homes to maintain a stock of PPE (including gloves, surgical masks, N95 masks, hand sanitizer, booties, etc.), with state inspections and financing mechanisms to allow all homes to obtain it.
- Testing: Pioneer called for regular COVID-19 point-in-time and surveillance testing among all nursing home residents and staff, including antibody testing for homes with significant outbreaks as needed.
- Reducing spread: Pioneer urged requiring nursing homes to demonstrate their ability to form isolation units with adequate numbers of beds for infectious onslaughts as a prerequisite for continued operation.
The Boston Globe’s recent Spotlight Team coverage of COVID-19’s impact on nursing homes prominently quoted Pioneer Institute’s Barbara Anthony, who noted, “Holyoke was a microcosm.” The problem here is broad and continuing. Pioneer has been actively involved in this crucial topic from the start and will continue to advocate on behalf of Massachusetts elders and their families.
Below, we share more details about the problems identified, and the proposals prepared, by Pioneer staff around these issues. This list is illustrative, not exhaustive – and there is more to come.
- Mary Connaughton’s April 17 blog, “Transparency Needed at Long-Term Care Facilities” was an early warning of the pandemic’s outsized impact in Massachusetts eldercare facilities, and an early call for transparency.
- On April 20, Andrew Mikula’s blog, “Elderly People Were Already Vulnerable to COVID-19. Then it Came to Nursing Homes” again warned of the pandemic’s growing threat to Massachusetts eldercare facilities – “Senior living facilities are uniquely vulnerable to this pandemic,” it stated — and proposed concrete improvements, including staff education, isolation of residents, and reconfiguration of common areas.
- On May 18, Greg Sullivan and Andrew Mikula’s report titled “Understaffing at Long-Term Care Facilities is Not Unique to the Holyoke Soldiers’ Home. It’s Embedded in Federal Standards” diagnosed an important cause of the tragedy at the Holyoke Soldiers’ Home — weak federal staffing standards. This report received extensive coverage by, among others, the Boston Herald and MassLive, with related coverage quoting Greg Sullivan in outlets including WHDH and WCVB.
- Barbara Anthony and Mary Connaughton’s May 20 WGBH Op-ed underscored deepening severity of the crisis, warned of “limited transparency,” and called for answers to core questions including “who in state government was/is in charge of the health and safety of long-term care facility residents and what lessons have been learned thus far?”
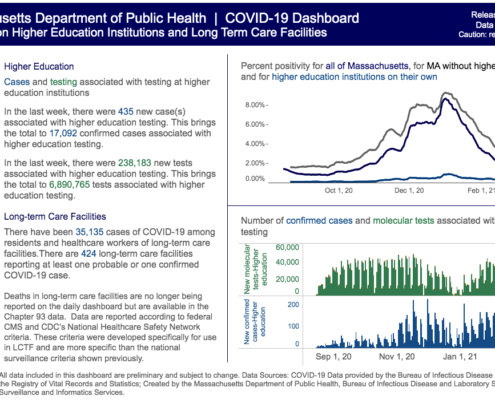
- On June 2 Pioneer directly enhanced transparency, launching its online COVID Tracker for Long-Term Care Facilities, which gives the public key data from the state’s weekly public health report for 320 eldercare facilities in a user-friendly format.
- On June 10, NECN/NBC Boston quoted Barbara Anthony on the “deplorable” failures to date, and the importance of changing course.
- On June 28, Barbara Anthony, Mary Connaughton and Andrew Mikula issued a 7-page open letter to the legislatively-created COVID-19 Task Force about “the unique vulnerability of nursing home residents to the Coronavirus.” Among much else, it suggested 14 practical, near-term fixes including the appointment of one person with “sole responsibility” for eldercare issues. The Globe dedicated an entire article to this open letter — “Group Calls for Urgent Nursing Home Reforms Amid COVID-19” – and then ran a July 5th Editorial which focused on the letter and its “promising” recommendations, again quoting Pioneer’s Barbara Anthony.
- August 11 brought Andrew Mikula’s account of a Pioneer records request for basic information about COVID-19 deaths among individuals with dementia in state-regulated facilities, which “potentially revealed shocking gaps in information on the facilities that the agency [DPH] oversees.”
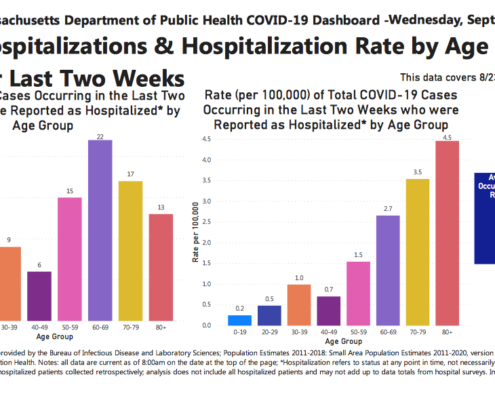
- David Clancy’s September 17 “A Step Backwards,” covered by the Boston Herald and the Berkshire Eagle, said the state is wrong to stop its daily reporting of cumulative data about the impact of COVID-19 on different age-groups, switching instead to weekly reports about age-group impact, based solely on the prior two weeks of data. The state should do both: report age-group impact on the basis of short-term data and cumulative data.
Get Our COVID-19 News, Tips & Resources!
Related Posts