
Do No Harm to the Health Policy Commission
With only weeks left in the Massachusetts legislative calendar,…
New Online Tool Tracks MA Hospital Revenue from Commercial Sources
A new online tool from Pioneer Institute shows a gradual increase in non-commercial (public payer) revenue at Massachusetts hospitals and also reveals a strong relationship between the hospitals with the highest commercial revenue and those with the highest relative prices.

Massachusetts Hospitals: Uneven Compliance with New Federal Price Transparency Law
A 2019 federal law requires hospitals to make prices for 300 shoppable services available online in a “consumer-friendly format,” but a Pioneer Institute survey of 19 hospitals finds that information on discounted cash prices—the price most likely to be charged to consumers paying out of pocket—was unavailable at seven of those hospitals.

Healthcare Price Transparency in Massachusetts: Results from a survey of Massachusetts consumers regarding healthcare price transparency
In June 2019, Pioneer Institute, with support from Blue Cross Blue Shield of Massachusetts and the Massachusetts Association of Health Plans, contracted with noted pollster David Paleologos, head of DAPA Research at Suffolk University’s Research Bureau, to conduct a valid and reliable survey of Massachusetts consumers with employer sponsored health insurance. The goals of the survey were to determine consumers’ awareness, attitudes, views, usage, and knowledge of healthcare prices. This white paper presents analysis of the results.
Analysis of Spending on Shoppable Services in Massachusetts
This report reveals that consumers in just one Massachusetts county could have saved nearly $22 million in a single year and $116.6 million adjusted for inflation over four years if they switched from using the most expensive providers for 16 shoppable healthcare services to those whose prices were closer to average.

Looming Challenges for ICER in Assessing the Value of Rare Disease Therapies
0 Comments
/
This report examines why the Institute for Clinical and Economic Review (ICER) and the Quality Adjusted Life Years (QALY) approach to value assessment is particularly ill-suited to assess the cost-effectiveness of orphan and rare disease treatments, which represent a rapidly growing sector of the biopharmaceutical marketplace.
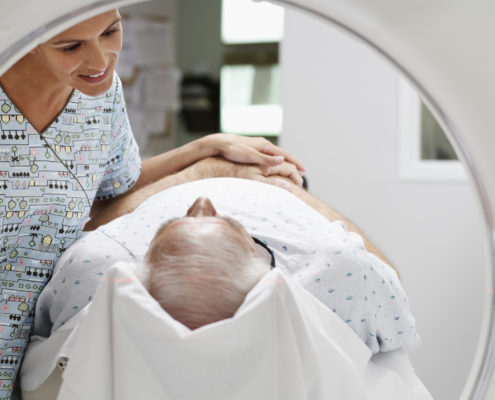
Wildly Varying MRI Prices at Massachusetts Hospitals: Why We Need Access to Healthcare Prices at All Levels
New study finds there is little correlation between a patient’s out-of-pocket cost and either the amount insurers pay or the overall price of a procedure at 14 representative Massachusetts hospitals.

Will New England See Lower Prices from Drug Pricing Transparency Legislation?
This report finds that most new drug pricing transparency laws do not lower consumer out-of-pocket costs, and that expensive and onerous compliance rules would likely put upward pressure on prices. The report reviews recent New England legislative attempts to reduce costs by requiring the disclosure of wholesale drug prices and other information about industry pricing practices.
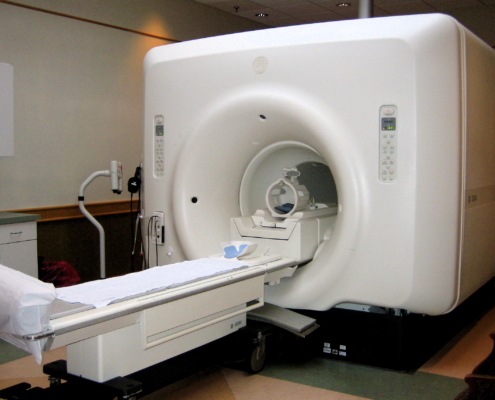
Need an MRI? In Worcester, Patients Pay Less for More
Data from the Massachusetts Center for Health Information and Analysis (CHIA) show wide variations in the prices agreed to between individual insurers and providers, the portion paid by insurers and the amount that is consumers’ responsibility to pay.

MA Health Insurers Have Improved Their Consumer Price Transparency Efforts, But Significant Work Remains
This study finds some significant improvements in the online cost estimator tools created by Massachusetts’ three largest health insurers, but there is much still to be done for the carriers to maximize the opportunity price transparency represents.

What Massachusetts Should Do in an Uncertain Healthcare World
Regardless of what happens in the debate over repealing and replacing the ACA in D.C., Massachusetts has to tackle health care costs intelligently. We need to do more than provide insurance; we need to increase access to care. That means thinking seriously about the role of private market insurers, insurance regulations and the regulation of medical providers.

Lowering the Healthcare Cost Growth Benchmark
This policy brief applauds the decision by the Commonwealth of Massachusetts's Health Policy Commission to allow the benchmark for increases in the overall rate of healthcare spending to decrease this year, but urges state policy makers to remain focused on the larger culture changes that will be needed to rein in healthcare costs.

Massachusetts Hospitals Score Poorly on Price Transparency…Again
Eighteen months after an initial survey of prices at hospitals in Massachusetts, Pioneer Institute conducted a follow-up survey of all but one of the hospitals from the first survey to see if there had been any change in the performance of these institutions since their last assessment. Initial survey calls were conducted between September 20th and November 2nd, 2016.

Recommendations to the Transparency Subcommittee of the Special Commission on Provider Variation
Submitted to the Special Commission on Provider Price Variation on January 31, 2017

Testimony on Healthcare Price Transparency
Testimony emphasized the need to focus more on what would help consumers make better decisions about spending on healthcare.

Over A Decade, The ACA Fee On MassHealth Will Cost Hundreds Of Millions Of Dollars
In “Over a Decade, the ACA Fee on MassHealth Will Cost Hundreds of Millions of Dollars,” authors Lauren Corvese and Josh Archambault examine the potential budget impact of the Health Insurer Provider Fee (HIPF), a revenue-raising mechanism for the Patient Protection and Affordable Care Act (ACA).

Healthcare Prices for Common Procedures Are Hard for Consumers to Obtain Survey finds hospitals not prepared to give price information to consumers
This policy brief is the third in a series of reports on healthcare price transparency prepared by Pioneer Institute. Researchers surveyed six major metropolitan areas and spoke with 54 acute care hospitals across those regions: Des Moines, IA, Raleigh-Durham, NC, Orlando, FL, Dallas-Ft. Worth, TX, New York, NY and Los Angeles, CA asking for the price of an MRI of the left knee without contrast. In addition, they explored the existence of federal and state laws that might apply in the states where the hospitals surveyed are located. They also examined the websites of the 54 hospitals for price information. The results of this survey are described in this policy brief.
What Will U.S. Households Pay for Health Care in the Future
This white paper reports that health care costs for a U.S. family of average income (including family insurance premium contributions and out-of-pocket costs including co-payments, coinsurance and deductibles) could increase from $8,583 annually to $13,213 by 2025, but up to as high as $18,251 in the same year. In terms of proportion of earnings, this would be equivalent to 20 percent and 27 percent of household income by 2025, respectively.

Bay State Specialists and Dentists Get Mixed Reviews on Price Transparency
Pioneer surveyed 96 specialists from across Massachusetts, split…

Mass Hospitals Weak on Price Transparency
Pioneer Institute surveyed 22 out of approximately 66 Massachusetts acute care hospitals and 10 free-standing clinics seeking prices for one common procedure - an MRI of the left knee without contrast. While Pioneer was ultimately able to get the information from all 10 clinics and 21 of the 22 hospitals, the process was time consuming, confusing and replete with long rounds of telephone tag.
The Undisclosed Cost of Developing an Affordable Care Act State Exchange in Massachusetts
The transition to the Affordable Care Act (ACA) in Massachusetts has been a bumpy one, to say the least. The state still lacks a functional website, and currently has almost 300,000 individuals on a newly created transitional Medicaid (MassHealth) program, with almost no program integrity provisions being observed, as little eligibility verification was run on the population upon enrollment.
Mayor, Tear Down This Wall: Why Boston’s Ban on Convenient Care Clinics Is Costing Taxpayers Millions
As convenient care clinics (also known as walk-in clinics or limited service clinics) grow in popularity across the nation, Boston remains empty of these clinics due to mayoral opposition. Convenient care clinics, a relatively new development in the world of health care, first emerged just 12 years ago.

New ACA Medicare Payroll Tax Hits Massachusetts, $1.7 Billion Over 10 Years
This brief is part of an occasional series from Pioneer Institute examining the direct effects of the ACA on Massachusetts. Please see the end of the paper for more examples.

Consumer Driven Health Care: A New Agenda for Cost Control in Massachusetts
This paper provides a discussion of CDHC, what it is and how it can help constrain health care costs and increase patient engagement in Massachusetts. While supply-side approaches are also necessary for cost control, without engaged consumers, Massachusetts may find that it cannot accomplish its cost-containment goals as quickly or as successfully as desired.

Impact of the Federal Health Law’s “Cadillac Insurance Tax” in Massachusetts
The Obama administration has done its best to highlight some of the more popular provisions of the law such as expanded preventative benefits, allowing children up to age 26 to remain on their parents insurance, closing the prescription drug “doughnut hole” for seniors on Medicare, and expanded contraception coverage. Yet, many of the less attractive provisions have not been given a local spotlight. This brief will examine the impact of the so-called “Cadillac tax” included in ObamaCare.

An Interim Report Card on Massachusetts Health Care Reform: Part 4
This report is the final report in a series of four. Earlier reports in this series evaluated access to health insurance and health care, equitable and sustainable financing, and administrative efficiency. The focus of this report will be on cost-effective quality, and the analysis will be organized by the four "Scorecard Metric,' presented in Figure 1.

An Interim Report Card on Massachusetts Health Care Reform: Part 3
This report is the third in a series of four. The focus of this report is on administrative efficiency.
An Interim Report Card on Massachusetts Health Care Reform: Part 2
As an alternative to analyzing the reform’s impact on isolated issues, in January 2009 the Pioneer Institute proposed a framework for evaluating the reform.

An Interim Report Card on Massachusetts Health Care Reform: Part 1
The focus of this report is on the reduction of barriers to access.

Drawing Lessons: Different Results from State Health Insurance Exchanges
Policymakers are considering several options for national health reform, each of which includes some form of "insurance exchange." These exchanges allow the uninsured, and employees of small to medium-sized businesses, to compare qualified health plans, purchase insurance and, if eligible, receive subsidies toward the cost of their plans.
